Refurbished Medical Devices
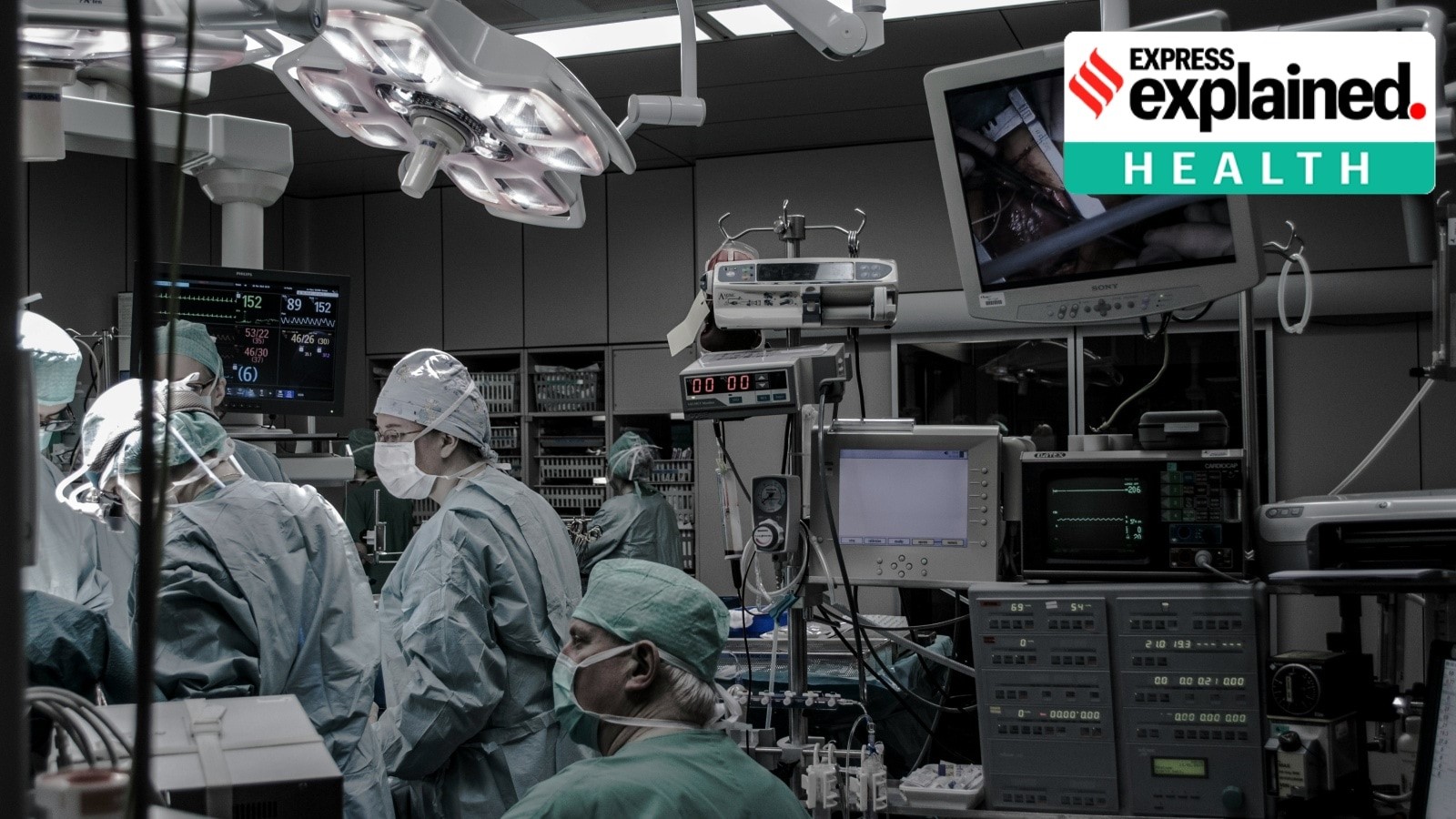
- 16 Feb 2026
In News:
The Government has constituted a committee under the Ministry of Health and Family Welfare (MoHFW) to draft a comprehensive policy on refurbished medical devices. The panel will define their scope, establish safety and performance assessment mechanisms, determine remaining useful life, and recommend disposal standards. The core policy challenge is not whether refurbished devices should be permitted, but how to regulate them while balancing healthcare affordability, patient safety, and Make in India objectives.
What are Refurbished Medical Devices?
Refurbished devices are previously used medical equipment restored to original operating standards and resold at lower prices.
They primarily include high-value capital equipment such as:
- MRI machines
- CT scanners
- PET-CT systems
- Robotic surgical systems
- Advanced endoscopy units
Cost Advantage (Key Data)
- 1.5T MRI:
- New: ?4–8 crore
- Refurbished: ?1–3.5 crore
- PET-CT system:
- New: ?20 crore
- Refurbished: ?60 lakh–3.5 crore
- CT scanner:
- New: ?2–4 crore
- Refurbished: ?20 lakh–2.5 crore
These price differentials significantly enhance diagnostic access in Tier-2 and Tier-3 cities, district hospitals and standalone centres, supporting decentralisation of healthcare.
India’s Import Dependence
Despite growth under Make in India, India remains dependent on imports for advanced imaging technologies due to technological complexity and global supply chain dominance.
Refurbished equipment is typically sourced from US, Germany, Japan and the Netherlands, where hospitals upgrade systems before end-of-life.
- Estimated size of refurbished segment: ?1,500 crore
- Share of total medical equipment market: ~10%
- Total medical device imports (last year): ?76,000 crore
- Medical electronics imports: ?48,000 crore
Current Regulatory Framework: Policy Gaps
1. Absence of Dedicated Pathway
- No separate licensing provision under Medical Devices Rules, 2017.
- All devices notified as “drugs” in 2020, but refurbished category undefined.
- No statutory distinction between “used,” “refurbished,” “reconditioned,” or “remanufactured.”
2. Governance under Waste Rules
Imports are regulated primarily under the Hazardous and Other Wastes (Management and Transboundary Movement) Rules, 2016.
Clearances required from:
- MoEFCC (expert committee)
- CDSCO (technical inputs)
- DGFT (import authorisation)
In December 2022, import of certain high-end used equipment was permitted under strict conditions.
3. Regulatory Conflict
- November 2025: MoEFCC approved several refurbished devices for reuse.
- January 2025: CDSCO stated refurbished devices cannot be imported for sale due to absence of licensing provisions.
This created legal inconsistency between environmental and medical device regulators, raising concerns over policy coherence and patient safety.
Industry Divide: Competing Perspectives
International Manufacturers (MTAI)
- Oppose blanket bans.
- Advocate regulated imports aligned with global standards.
- Argue refurbished devices improve affordability, training access, and complement industrial initiatives like Electronics Repair Services Outsourcing.
Domestic Manufacturers (AiMeD)
- Seek strong regulatory safeguards benchmarked to global norms.
- Raise concerns over:
- Unclear usage history
- Limited traceability
- Shorter lifespan
- Risk of India becoming a dumping ground for end-of-life equipment
- Estimate ?12,000–15,000 crore unauthorised trade in pre-owned devices.
Core Policy Dilemma
India faces a three-way balancing act:
- Healthcare Access – Affordable diagnostics for smaller cities.
- Patient Safety & Regulatory Oversight – Clear licensing, traceability, lifecycle standards.
- Industrial Self-Reliance – Protecting domestic innovation and long-term technological capability.
Way Forward
A coherent policy must:
- Define refurbished categories clearly.
- Establish lifecycle assessment and certification standards.
- Align with global regulatory benchmarks.
- Ensure OEM accountability and service traceability.
- Integrate environmental, trade and health regulations into a unified framework.
A balanced regulatory model can simultaneously expand access to advanced diagnostics and strengthen India’s ambition for technological self-reliance in medical devices, aligning public health priorities with industrial development.
